When it comes to toileting habits, the topic is not exactly a favorite among Americans – at least for those above the age of four. Mention poop and you can easily clear a room – or at the least, generate some unusual facial expressions, nervous laughter, and wisecracks about “too much information.”
But your bodily emissions are an important health topic that deserves serious attention, regardless of the “ick factor.” In fact, if you ignore what you deposit in your toilet, you could be flushing your health down the drain!
Did you know the average person generates about five TONS of stool in his or her lifetime? Turns out, there is much to be learned from this mountain of poop.
The shape, size, color, and other fecal features can tell you a great deal about your overall health, how your gastrointestinal tract is functioning, and even give you clues about serious disease processes that could be occurring, like infections, digestive problems, and even cancer. Poop comes in just about all the colors of the rainbow… and please forgive me for using the words poop andrainbow in the same sentence.
Although there is a certainly a wide variety of stool colors, textures and forms that are considered “normal,” there are definitely things that, if seen or experienced, warrant immediate medical attention. With this in mind, the overview that follows covers what you need to know about what’s normal and not normal in the bathroom department.
What is Normal Stool?
Your stool is about 75 percent water. The rest is a fetid combination of fiber, live and dead bacteria, miscellaneous cells and mucus.1, 2 The characteristics of your stool will tell you a good deal about how happy and healthy your digestive tract is – the color, odor, shape, size, and even the sound it makes when it hits the water and whether it’s a “sinker” or a “floater” are all relevant information.
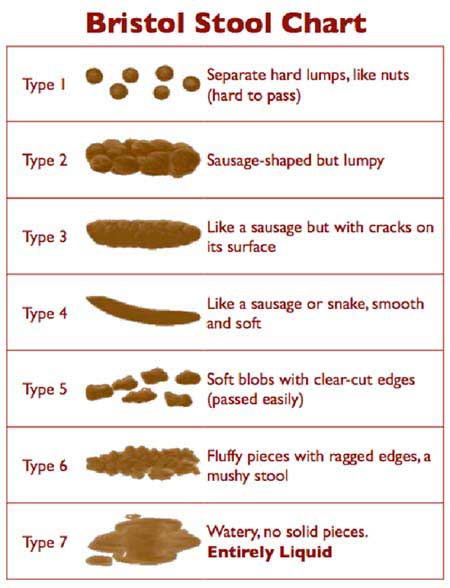
The Bristol Stool Chart is a handy tool that may help you learn what you’re going for. Ideally, your stool should approximate Types 3, 4 and 5, “like a sausage or a snake, smooth and soft” to “soft blobs that pass easily.” Type 4 is the Holy Grail.3
Fiber tends to bulk up your stool and acts like glue to keep the stool stuck together, instead of in pieces. If your stool is on the softer side, short of diarrhea (“soft serve,” as some call it), it could be related to lactose intolerance, artificial sweeteners (sorbitol and Splenda), or a reaction to fructose or gluten.
Look, Listen and Smell Before You Flush
What’s normal and what’s not when you look into the toilet? The following table will help you narrow down what to look for, so that you aren’t needlessly alarmed. Of course, there are a few signs that ARE cause for concern, and those are listed too. If you have a change in stools accompanied by abdominal pain, please report this to your physician.4
Healthy Stool Unhealthy Stool Medium to light brown Stool that is hard to pass, painful, or requires straining Smooth and soft, formed into one long shape and not a bunch of pieces Hard lumps and pieces, or mushy and watery, or even pasty and difficult to clean off About one to two inches in diameter and up to 18 inches long Narrow, pencil-like or ribbon-like stools: can indicate a bowel obstruction or tumor – or worst case, colon cancer; narrow stools on an infrequent basis are not so concerning, but if they persist, definitely warrant a call to your physician5 S-shaped, which comes from the shape of your lower intestine6 Black, tarry stools or bright red stools may indicate bleeding in the GI tract; black stools can also come from certain medications, supplements or consuming black licorice; if you have black, tarry stools, it’s best to be evaluated by your healthcare provider Quiet and gentle dive into the water…it should fall into the bowl with the slightest little “whoosh” sound – not a loud, wet cannonball splash that leaves your toosh in need of a shower White, pale or gray stools may indicate a lack of bile, which may suggest a serious problem (hepatitis, cirrhosis, pancreatic disorders, or possibly a blocked bile duct), so this warrants a call to your physician; antacids may also produce white stool Natural smell, not repulsive (I’m not saying it will smell good) Yellow stools may indicate giardiainfection, a gallbladder problem, or a condition known as Gilbert’s syndrome – if you see this, call your doctor Uniform texture Presence of undigested food (more of a concern if accompanied by diarrhea, weight loss, or other changes in bowel habits) Sinks slowly Floaters or splashers Increased mucus in stool: This can be associated with inflammatory bowel disease like Crohn’s disease, or ulcerative colitis, or even colon cancer, especially if accompanied by blood or abdominal pain
Does Your Stool Have a Really Bad Odor?
If your stool has an extraordinarily bad odor, it should not be ignored. I am referring to an odor above and beyond the normally objectionable stool odor. Stinky stool can be associated with a number of health problems, such as:7
- A malabsorptive disorder
- Celiac disease
- Crohn’s disease
- Chronic pancreatitis
- Cystic fibrosis
Cystic fibrosis (CF) is a disease caused by a defective gene that causes your body to produce abnormally thick, sticky mucus, which builds up and causes life-threatening lung infections and serious digestive problems. Most cases of CF are diagnosed before the age of 2, so this is more of a concern with infants and toddlers.
Speaking of malodorous things, what about gas? Passing gas (flatulence) is normal. Not only is it normal, it’s a good sign that trillions of hard working gut bacteria are doing their jobs. People pass gas an average 14 times per day – anywhere from one to four pints of it!8 Ninety nine percent of gas is odorless, so you may even be unaware you’re passing it. Think about it – were it not for an exit, we’d all blow up like balloons!
How Often Should You Move Your Bowels?
Normal bowel habits vary. When we talk about regularity, what we’re really talking about is what’s regular for you. Three bowel movements per day to three per week is considered the normal range.
What’s more important than frequency is the ease with which you move your bowels. If you need to push or strain, something is off – moving your bowels should take no more effort than urinating or passing gas. The thing to watch for is a sudden change in your bowel habits. Many factors can affect regularity, such as diet, travel, medications, hormonal fluctuations, sleep patterns, exercise, illness, surgery, childbirth, stress and a whole host of other things.9
Constipation and Diarrhea
The average body takes between 18 and 72 hours to convert food into poop and pass it on out. When this time is significantly shortened, the result is diarrhea because your intestine doesn’t have time to absorb all of the water. Conversely, when transit time is lengthened, you may end up constipated because too much water has been absorbed, resulting in hard, dry stools.
Constipation is defined as passing hard, dry stools that you have to strain to move, and it’s typically accompanied by decreased frequency of defecation. Straining is not normal, nor are experiencing feelings of incomplete elimination, bloating, crampiness, or sluggishness after going number two. If you’re over the age of 65, your risk of becoming constipated increases significantly.
Chronic, untreated constipation can lead to fecal impaction,10 which can be a serious medical condition. Laxatives should be avoided at all cost and used only as a last resort. If you absolutely must use a laxative, make sure it is used for only a very short period of time.
Common Causes of INCREASED Bowel Frequency/Diarrhea11 Lifestyle Diseases and Conditions Eating more fruits and vegetables (increased fiber) Hyperthyroidism (overactive thyroid) Increased exercise Crohn’s disease Drinking more water Ulcerative colitis Emotional stress Celiac disease Food allergies Irritable bowel syndrome (IBS) Medication side effects Gastrointestinal infection Common Causes of DECREASED Bowel Frequency/Constipation12, 13 Change in diet, less fiber, less fruits and vegetables Pregnancy, childbirth, or hormonal disturbances Emotional stress Problems with the muscles or nerve in the intestine, rectum or anus Ignoring the urge to “go,” travel and scheduling factors that cause you to hold it Irritable bowel syndrome (IBS) Insufficient exercise Diabetes Inadequate hydration Hypothyroidism (underactive thyroid) Calcium or iron supplements Local pain or discomfort around the anus, such as from fissures or hemorrhoids Drugs such as narcotic painkillers (codeine, for example), diuretics, antacids, antidepressants, and excess or overused laxatives Less often: diverticulitis, intestinal obstruction, colorectal cancer, multiple sclerosis, Parkinson’s disease and spinal cord injury Food allergies
How to Score a Home Run with Your Bowel Movements
Most gastrointestinal problems can be prevented or resolved by making simple changes to your diet and lifestyle. If you aren’t achieving poo perfection, or if you don’t feel right, then look at the following factors and consider making a few changes. These strategies will help reverse constipation or diarrhea, in addition to helping prevent recurrences.
- Remove all sources of gluten from your diet (the most common sources are wheat, barley, rye, spelt and other grains)
- Eat a diet that includes whole foods, rich in fresh, organic vegetables and fruits that provide good nutrients and fiber; most of your fiber should come from vegetables, not from grains
- Avoid artificial sweeteners, excess sugar (especially fructose), chemical additives, MSG, excessive amounts of caffeine, and processed foods as they are all detrimental to your gastrointestinal (and immune) function
- Boost your intestinal flora by adding naturally fermented foods into your diet, such as sauerkraut, pickles, and kefir (if you tolerate dairy); add a probiotic supplement if you suspect you’re not getting enough beneficial bacteria from your diet alone
- Try increasing your fiber intake; good options include psyllium and freshly ground organic flax seed (shoot for 35 grams of fiber per day)
- Make sure you stay well hydrated with fresh, pure water
- Get plenty of exercise daily
- Avoid pharmaceutical drugs, such as pain killers like codeine or hydrocodone which will slow your bowel function, Antidepressants, and antibiotics can cause a variety of GI disruptions
- Address emotional challenges with tools like EFT
- Consider squatting instead of sitting to move your bowels; squatting straightens your rectum, relaxes your puborectalis muscle and encourages the complete emptying of your bowel without straining, and has been scientifically shown to relieve constipation and hemorrhoids
CLICK HERE to Pin this post
Original Source: Mercola










3 Replies to “What You See in the Toilet Can Give You Valuable Insights into Your Health”